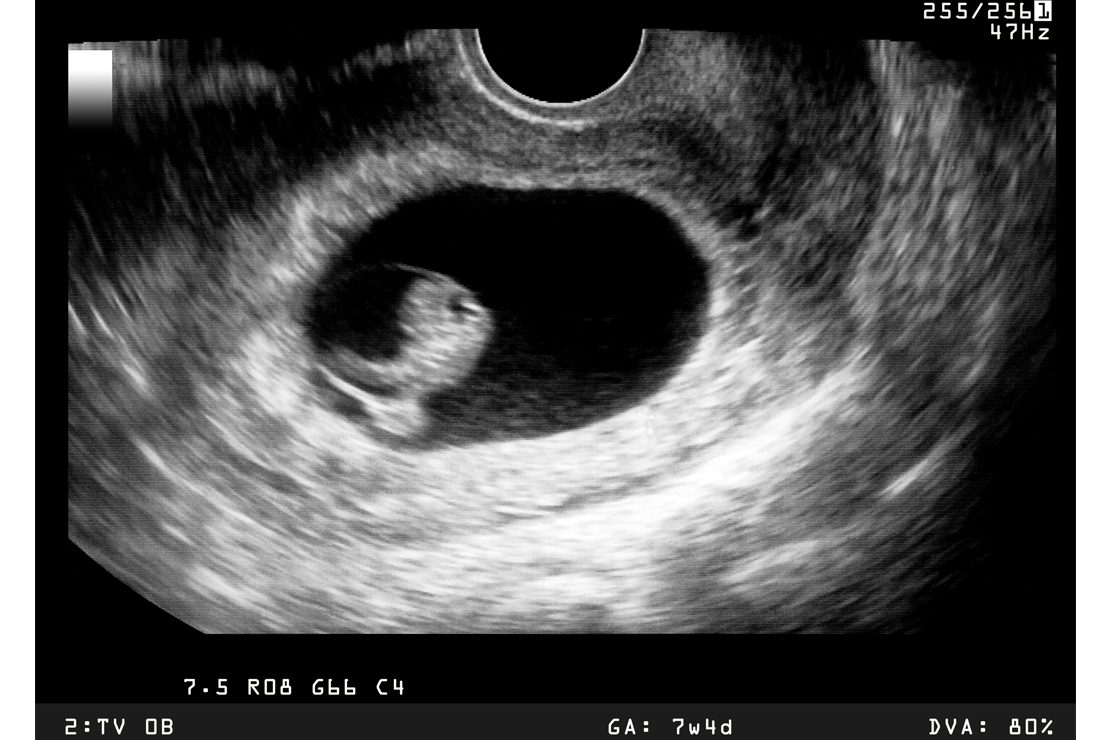
非存活妊娠详解:原因、症状和后续步骤
介绍
许多人在接受生育治疗或早期妊娠检查时都会遇到“非存活妊娠”这个词 。听到这个词可能会让人感到困惑和情绪崩溃,尤其是对于那些正在尝试通过试管婴儿或代孕受孕的人来说。
患者经常搜索“非存活妊娠的含义”、“什么是非存活妊娠”以及“非存活妊娠的迹象”等信息, 以寻求更清晰的了解。了解这一诊断的意义、发生原因以及后续可选择的方案,可以帮助患者在获得更多知识和支持的情况下应对这种情况。
什么是非存活妊娠?
非存活妊娠是 指无法继续发育并最终分娩的妊娠。医学上讲,这意味着胚胎或胎儿无法在子宫外存活,也无法正常发育。
该术语通常用于早期妊娠评估,当医学检测表明发育已经停止或无法安全继续时使用。
医生可以通过以下方式判断妊娠是否无法继续:
• 超声成像
• 激素水平监测
• 无胎心搏动
• 胚胎发育异常
因此, “非存活妊娠”一词指的 是不幸无法继续妊娠直至健康分娩的情况。
常见的非存活妊娠类型
多种情况都属于非存活妊娠的范畴。
其中包括:
• 早期妊娠丢失或流产
• 空孕囊(无胚胎妊娠)
• 异位妊娠
• 严重的染色体异常
每种疾病的病因各不相同,但都会导致妊娠无法正常发育。
非正常妊娠的迹象
早期症状可能因人而异。有些人很快就能注意到身体的变化,而有些人则是在例行体检时才发现自己患有这种疾病。
妊娠失败的常见迹象 可能包括:
• 阴道出血
• 痉挛或腹痛
• 减轻妊娠症状
• hCG激素水平缓慢上升或下降
• 超声检查显示无胎心搏动
然而,需要注意的是,仅凭症状并不能确诊。只有医学评估才能确定妊娠是否可行。
医生如何诊断非存活妊娠
医生依靠多种诊断工具来确认妊娠是否成功。
最常用的方法是进行非妊娠超声 评估。
在超声检查过程中,医生可能会观察到:
• 无发育中的胚胎
• 妊娠囊但无胎儿发育
• 妊娠期未见胎心
• 异常生长模式
血液检测(测量 hCG 激素水平)也可用于追踪妊娠进展。
当激素水平没有适当上升或超声检查结果显示发育停止时,医生可能会诊断为非存活妊娠。
导致妊娠失败的原因
大多数无法存活的妊娠是由于早期胚胎发育过程中染色体异常造成的。这些遗传问题随机发生,通常与父母的任何行为无关。
其他可能的原因包括:
• 胚胎染色体异常
• 激素失衡
• 子宫结构异常
• 严重的植入问题
• 孕产妇健康状况
在试管婴儿等生育治疗中,对胚胎进行基因检测可能有助于降低某些染色体问题的风险。
试管婴儿和代孕中的非存活妊娠
辅助生殖治疗期间也可能发生非正常妊娠。即使采用先进技术,早期妊娠丢失仍然存在可能。
在体外受精或妊娠代孕案例中,医疗团队通过超声波和激素检测密切监测妊娠情况。
如果在代孕过程中出现无法存活的妊娠,专业人员会与准父母和代孕母亲合作,确定最安全的后续医疗措施。
像云达代孕中心这样经验丰富的机构 会为面临此类情况的家庭提供支持,包括协调医疗指导、情感支持和后续计划。他们的职责通常包括帮助准父母了解各种治疗方案,并为未来可能的胚胎移植做好准备。
非正常妊娠后会发生什么
当确诊为非妊娠性妊娠时,医生会讨论几种医疗方案。
这些可能包括:
• 期待疗法(等待自然流产)
• 辅助流产的药物
• 诸如刮宫术之类的小型外科手术
推荐方案取决于医疗安全性和患者意愿。
情感影响和支持
妊娠失败带来的情感冲击可能非常巨大。患者可能会经历悲伤、困惑或沮丧,尤其是在接受过生育治疗的情况下。
支持资源可能包括:
• 咨询服务
• 生育支持小组
• 为后续治疗提供医疗指导
• 与护理团队沟通
正视生育挑战带来的情感困扰是康复的重要组成部分。
非存活妊娠后的未来生育能力
经历过一次非正常妊娠并不意味着以后就不可能怀孕。许多人之后都能成功怀孕。
医生可能会建议:
• 基因检测
• 激素评估
• 子宫成像
• 体外受精方案的调整
了解根本原因有助于指导未来的生育计划。
常见问题解答
非存活妊娠是什么意思?
它指的是由于医疗或发育问题而无法继续发育为活产的妊娠。
无法存活的妊娠有可能转为可存活吗?
不。一旦医学上确诊妊娠无法继续,胎儿就无法正常发育。
非存活妊娠是否意味着流产?
通常是这样。许多无法存活的妊娠最终会导致流产,尽管有时可能需要药物治疗。
结论
得知妊娠无法继续进行,对患者来说可能是一件非常痛苦和艰难的事情。了解妊娠无法继续进行的含义、原因和医疗选择,有助于患者更清晰地应对这一经历。
即使在严密监控的生育治疗中,早期妊娠流产也可能发生,但这并不影响未来的成功。在适当的医疗护理、情感支持以及像云达代孕这样经验丰富的专业人士的指导下,许多家庭能够重拾希望,继续他们的为人父母之路。
